Using the Hierarchy of Controls to Reduce Exposure to COVID-19
By Newfront | Published April 17, 2020

As an industrial hygienist, I wanted to discuss how to reduce the spread of disease in your workplace using the Hierarchy of Controls model – typically used to evaluate and prioritize risk control solutions to maximize effectiveness and feasibility.
The Hierarchy of Control model, for risk reduction and control, was first introduced in 1950 by the National Safety Council with the simple philosophy of “Controlling exposures to occupational hazards is the fundamental method of protecting workers”. During our current emergency, employers must reevaluate exposures and develop new ways of reducing the risks to our employees. Because employers are experiencing significant issues locating PPE for use in the workplace, the Hierarchy of Controls should be used to evaluate and develop a comprehensive risk reduction strategy.
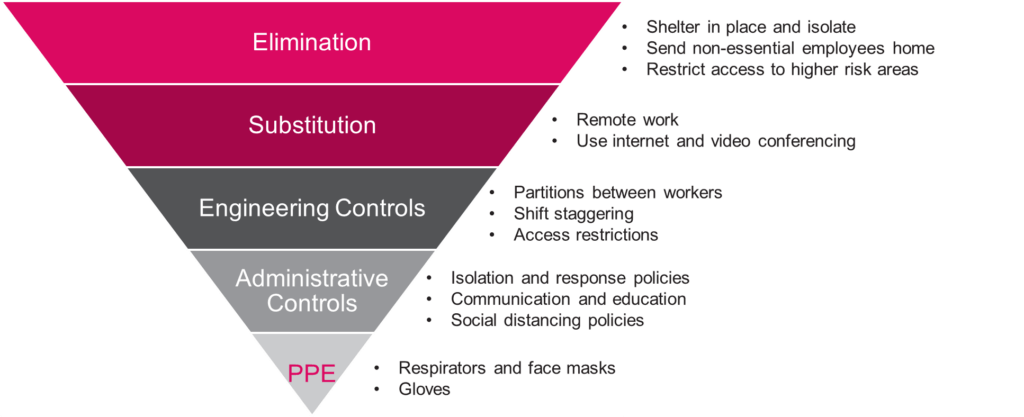
The inverted triangle represents a typical model, with control methods at the top that are the most effective and protective, down to the least protective or efficient controls at the bottom.
Recently, the Occupational Safety and Health Administration (OSHA) has been in the news discussing the use of non-medical masks while in public, as per CDC recommendations. However, OSHA is warning employers that these non-medical or non-NIOSH approved masks are not enough to keep some essential workers safe in certain occupations. Medical facilities around the country are already having a hard time securing adequate supplies of respirators and gloves which means many employers are having an even harder time acquiring needed safety equipment. Because of this, OSHA has been loosening their own requirements, but they expect to find other controls in their place.
OSHA is maintaining a priority for medical grade or NIOSH-certified respirators for medical facilities in their guidance. Employers must look to the hierarchy of controls to develop effective control measures before solely relying on personal protective equipment (PPE).
When using the model, you first need to identify the tasks and hazards to which employees are exposed. Exposures will vary depending on the workplace and task, and therefore require a different evaluation process. Reviewing each work task and its potential exposure to disease is critical to identify all possible transmission routes and potential risk control methods. Starting at the top, with the hazard identified, you attempt to control the hazard based on that level. If the prevention method is not possible, you move down to the next levels. In many cases, there may be a combination of methods with the priority for control always starting at the top of the inverted triangle.
The following is an explanation of each of the levels of the model and how they would apply to protecting your employees from COVID-19.
Elimination and Substitution
Elimination and Substitution are the most effective at reducing exposure to COVID-19. However, they tend to be the most difficult to implement and make it challenging to get work done. Essentially, at this level, it means complete isolation from the outside world, staying home and staying safe by following local health departments shelter-in-place orders. The problem with this level is, those classified as essential employers must keep working, and elimination and substitution may not be possible. However, if we have employees who are not necessary on-site, they should stay home – we can essentially eliminate their exposure from the workplace. Substitution in the case of COVID-19 exposure prevention would be substituting the normal work environment for a safer one. This might include the employees’ home or a restricted access area of your facility. Elimination and substitution would also apply to controlling the introduction of the virus into the workplace. Restaurants, for example, have utilized these techniques by substituting pick-up-only food service for dining in.
Engineering Controls
Engineering controls are the next-most desired step in reducing exposure because they are designed to remove the hazard prior to coming into contact with the worker. These controls are typically very effective at protecting the worker and often do not rely on the worker activating or interacting with the control. You have most likely seen some of these controls already – many supermarkets have installed clear plexiglass panels above the checkout aisles. These reduce transmissions between customers and employees during checkout. In some cases, the initial cost of engineering controls will be higher than personal protective equipment such as masks, but the long-term effectiveness and lack of need for employee interaction provides cost savings over time. Other engineering controls include:
Increasing space between workstations or customers
Adding partitions between workstations or between customers
Increasing air flow from the outside by increasing the percentage of outside air to your HVAC system. (You may need to contact your HVAC contractor to make this change.)
Administrative Controls
For COVID-19 exposures, administrative controls can offer a lot of opportunities for exposure reduction. These types of controls involve changes to procedures, behaviors, and policies. Essentially, we are focused on changing how work is done. These solutions tend to be more expensive and difficult to implement, but they also are a great way to reduce exposures without resorting to personal protective equipment in some exposures. For reduction of exposure to COVID-19, controls include social distancing policies, such as reducing the number of workers on a shift, adding shifts, and staggering their start and end times to reduce the number of workers in the building. Other controls include:
Identification and isolation policies for suspected or confirmed COVID-19 cases
Response protocol for confirmed or suspected cases that includes facility disinfection procedures
Worker education on social distancing and ways they can reduce the spread of the disease
Ensuring that sick leave policies are flexible and do not encourage sick workers to come to work
Reduce or eliminate face to face meetings. Use the telephone or video conferencing
Provide hand sanitizer and tissues at all building entrances
Provide sanitizing wipes for all regularly used surfaces with a policy of frequent disinfection
Provide soap and water for frequent hand washing
Communication with employees through posters, web meetings, phone calls that encourage hand hygiene, social distancing and when to notify that you might be sick
Discourage hand shaking and promote other methods such as the virtual high five
Delivery or pick-up of product to curb-side or non-contact delivery methods
Restricting access to your facility to essential employees only
Personal Protective Equipment
Personal protective equipment is the last, and least overall effective, option. As we move down the inverted triangle, the effort and interaction of the worker become more prominent. For example, the use of a respirator requires an employee to properly put it on, make sure it is working and maintain it. This requires training, coaching, and oversight of the employee. The added complexity of employee involvement can reduce the overall effectiveness of the control and increase costs over time. For COVID-19, the use of respirators has been recommended by the CDC, but supplies are diminished, and many employers cannot obtain the needed equipment. Depending on the exposure, the use of non-medical or non-NIOSH certified face coverings mean employees are potentially not protected from exposure. The use of the higher levels of the Hierarchy of Controls model including elimination and engineering controls and the numerous administrative controls should all be implemented prior to depending on PPE. However, many counties have now issued requirements for people to wear masks while outside of their homes including while at work. Depending on your county Department of Health Orders, you may need to mandate the use of face coverings in your workplace. The CDC’s website has a guide that covers face covering recommendations and how to make them if they cannot be purchased.

Newfront
Newfront is a modern brokerage transforming the risk management, business insurance, total rewards, and retirement services space through the combination of elite expertise and cutting-edge technology. Specializing in more than 20 industries and headquartered in San Francisco, Newfront has offices nationwide and is home to more than 800 employees serving organizations across the United States and globally.